Health & Wellness
Grappling with the Opioid Crisis
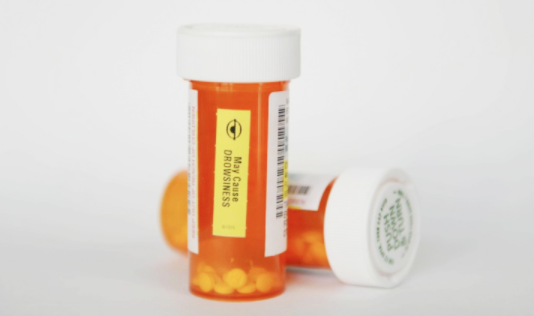
Opioid use and its addiction have swept through the United States in recent years. This tidal wave of misery has been left unchecked due to the stigma of drug dependency. While social drinking and recreational drug use are common in this country, once someone crosses the addiction line, support and understanding dwindles. In the PBS documentary, “Understanding the Opioid Epidemic,” that aired February 18, 2018, it is revealed that “opioid drug overdose is now the leading cause of death for people under the age of 50.”
The Centers for Disease Control and Prevention stated recently “the opioid epidemic is fueled by prescription pain medication.” To study the crisis from a local vantage point, this reporter contacted hospitals that serve Central Brooklyn. It is the senior medical staff at Interfaith Medical Center that participated in the interview. The two main contributors were Dr. Jason Hershberger, Chairman of Psychiatry at Interfaith Medical Center and Brookdale University Hospital and Medical Center, and Ms. Sharonie Perry, Director of Community Affairs at Interfaith Medical Center, with contributions from Dr. LaRay Brown, CEO of Interfaith Medical Center; Dr. Susan Kleinrock, Deputy Director at NYC Health and Hospitals Corp., and they responded to the following questions in one voice.
- Does Interfaith Medical Center (Interfaith) maintain statistics on patient (outpatient or admitted) opioid dependency? If yes, what do the numbers reveal?
While the Borough of Brooklyn, as a whole, ranks 3rd in the number of deaths due to drug overdose and emergency visits caused by opioids (after Staten Island and the Bronx), the problem of substance abuse is very high in our local neighborhoods. The NYC Department of Health and Mental Hygiene reports that people living in Crown Heights, Prospect Heights and Bedford-Stuyvesant are hospitalized due to alcohol problems at a rate 1.5 times higher than the rest of Brooklyn. Drug-related hospitalizations are double the borough average.
What this means is that safety-net hospitals like Interfaith are working twice as hard to save lives from the ravages of addiction, and our communities are suffering a disproportionate burden of this problem.
2) What are treatment options for opioid addiction?
There are several treatment options and Interfaith has a large number of programs to help. We provide inpatient detoxification services for patients in acute danger of overdose or withdrawal. We provide 14-28-day inpatient rehabilitation to help start patients on the path to recovery. We provide intense outpatient services focused on chemical dependency to help patients avoid relapse. We provide a methadone clinic to help patients with medication to avoid the perils of addiction and to stabilize their lives. We are opening a medication-assisted treatment program integrated into our Bishop Walker Primary Care Clinic to help patients with drug and alcohol problems using cutting-edge treatments like Buprenorphine and Naltrexone.
3) Is there a particular section of the brain that opioids stimulate that makes long-term recovery challenging?
Yes, there are several areas of the human brain that get ensnared in addictions. Our brains are designed to repeat behaviors that are rewarding, and drugs trick the brain into believing that really destructive behavior is good for us. Different drugs impact different parts of our brains, but all of them result in this same problem: the drugs make people feel like everything is great when life is really crashing around them.
4) In the one-hour PBS documentary, “Understanding the Opioid Epidemic,” it is explained that pharmaceutical companies marketed opioids to physicians as “safe, not addictive, and effective for pain management.” Did Interfaith Medical Center receive such marketing? If yes, what was the response?
We haven’t seen this documentary, but there certainly was a period in America when pharmaceutical companies promoted pain management strategies that helped bring about this epidemic. But Interfaith has always put patient care first. That means making responsible medical judgments and helping patients achieve pain relief while steering them away from the risks of addiction. That is why all Interfaith physicians check the pharmacy records of patients before we prescribe potentially addictive substances.
5) What are the alternatives to opioids–eg., hydrocodone and oxycodone–for managing pain? Are there any protocols that do not involve drugs?
There are many alternatives to opioids for pain relief. There are many non-opioid pain medications that can be very effective in some situations. There are also non-pharmacological approaches using physical therapy, massage, acupuncture and biofeedback that have good evidence behind them.
6) Is there evidence that suggests that opioids have surpassed crack cocaine in demand or do these two drugs operate in different social segments?
It depends on your perspective. From a nationwide perspective, opioids have definitely surpassed crack cocaine, but from a local perspective, and the perspective of most inner-city urban centers, crack cocaine remains a major problem. Sadly, the opioid epidemic is hitting us here in our neighborhoods while we are still grappling with the devastation of crack. 7) There are some in society who believe that opioid addiction is “an issue for white people.” Is there any truth to this thinking? No, opioid addiction doesn’t discriminate. It is hitting people of color, undermining our families, just as much as anyone.
8) Given the national epidemic, do you have an idea why there hasn’t been a massive march to decry prescribed opioids and street drugs? Sadly, we do. Fundamentally, it is the stigma our society puts on addictions that dulls the public outcry. If people were dying of the flu at the rates we are seeing people die of drug overdoses, it would be headline news every day. We applaud Our Time Press for picking up this story and pushing for more awareness, more communication, better public policy and more funding to address this scourge. 9) If you have concerns about prescription opioids that aren’t addressed in the above questions, please express your thoughts. Interfaith Medical Center is in the eye of the opioid crisis, one that has affected so many in our community. Interfaith has responded by educating its staff and the community about this important issue and has helped to develop innovative programs like the Anti-bullying Partnership for the Prevention of Violence and Suicide Prevention that has been working in conjunction with the Mayor’s Thrive NYC initiative and the New York City Department of Health and Mental Hygiene. The goal of this partnership is to offer preventive strategies that offer additional tools to local stakeholders, as well as to raise awareness in every sector of the neighborhood, from children to seniors. One such strategy is to provide staff and the community with Mental Health First Aid training. Individuals who complete the six-hour training receive a 3-year certification, as well as a Nasal Naloxone Injection Kit which is used to help revive an overdose victim. The opioid epidemic is a war that cannot be won unless groups and individuals come together to develop campaigns that will make a lasting impact. Interfaith has been in the forefront of forging coalitions throughout the community in order to eliminate this latest crisis. Interfaith is also participating in the Greater New York Hospital Association Opioid Advisory Workgroup. This workgroup is helping hospitals respond to the opioid epidemic by providing training programs for staff, helping staff connect individuals with addiction to treatment and treating chronic pain with individuals in recovery.